What a frustrating adventure to Denver! We did get to see our wonderful family... and that made the trip worthwhile. The study itself was ridiculous!
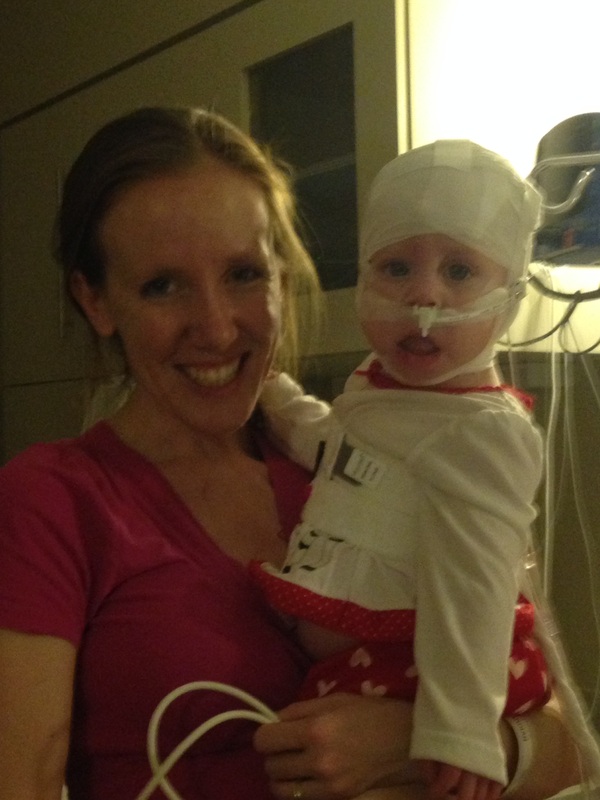
Our purpose of the study was to prove that the tongue reduction fixed the sleep apnea. It seemed to us that Kaylee's sleeping routine had improved since her surgery, and we rarely, if ever, catch her holding her breath any more. We arrived Friday, at 7:15pm, after Kaylee's normal bedtime. We got changed into her jammies and covered in sensors. They stuck 20 some odd sensors all over her head and under her chin to monitor brain activity... watching her sleep cycle. There were sensors stuck to her chest and legs to monitor activity. And she had an oxygen cannula in her nose, to provide oxygen (if needed) and it also provided some sort of suction to capture CO2, to monitor her CO2 output. Poor kid looked like a mummy once she was all ready for bed... see the picture below. Now I'm not sure how they expect anyone to sleep like this... and apparently their sensors also make it hard to breathe properly. When I was feeding Kaylee to put her to sleep, I told the lab tech that Kaylee's breathing sounded labored. She assured me it was fine and that this is the way they test all children. We were at the Children's Hospital, so I supposed they knew what they were doing. Kaylee was put in her crib, asleep, at about 9pm. She woke at 10, 11, and 12... very very unlike her. She would have normally slept until at least 1. And each time she woke, she was very upset. There were times she'd wake up gasping for air. She used to do that before tongue reduction and before oxygen... but hasn't done it since her surgery. Once she tried to push me away... my cuddling her was making her uncomfortable. For such a cuddle bug to be pushing me away, that was a huge red flag! At 1am, the tech came to turn Kaylee's oxygen on. Her oxygen saturation had been low. I was so angry to see this. I am fairly confident Kaylee doesn't need oxygen. She was having anything but a normal night. I pulled the nurse out, as to not wake Kaylee and told her my theory. To me it seemed that the gauze that was wrapped under her chin to hold sensors in place was just tight enough it was providing upward pressure on her jaw, closing it slightly. While this may be a natural position for most babies, Kaylee's tongue is still thick, so this was forcing her tongue back into her airway, creating... SURPRISE!... an obstruction. She tried to tell me that the way she was wrapped was standard procedure for all kids... I really should have pointed out that Kaylee isn't most kids... how often does she perform sleep studies on kids with macroglossia?! Anyway, I convinced her to clip the gauze that went under Kaylee's neck. An hour later, she admitted Kaylee was doing better (she sounded much better, but still labored), though couldn't say whether it was the gauze or the supplemental oxygen. There were times Kaylee would wake up gasping for air, and as she took a breath, I'd hear the suction release from the CO2 monitor... it was somehow sucking out air Kaylee was trying to breath. Yet another obstruction. And as minor as it may be, I feel like the elastic strap around her chest was adding extra compression, making it hard for her to take full breaths. Shallow breaths=low oxygen saturation levels. Needless to say, it was a very restless night. They only allowed one parent to stay in the room. They had high powered microphones on her crib to pick up her breathing, so they wanted to limit the extra noise. I was fuming mad watching how uncomfortable she was and how unwilling the tech was to help make her more comfortable or solve any breathing problems by removing sensors, or even allowing her to sleep on her stomach. Poor Ryan was getting bombarded with texts throughout the night as the study unfolded... or fell apart... however you want to look at it. Seeing as how the tech turned on her oxygen at 1am, I was certain the ear, nose, and throat (ENT) doctor we would be following up with would be sending us home with oxygen. This made us even more mad... that a study that in no way reflected her normal breathing habits would be the deciding factor between whether or not we had to mess with oxygen again. We went over every detail of what we thought went wrong and compared it to what normal looks like. I even called the nurse from St. Louis to confirm that the study seemed to be creating obstructions. She supported our observations and provided data to help make our case that she should be breathing better. When we saw the ENT, he had not yet reviewed the sleep study and asked our opinion. So I told it to him. Surprisingly, he listened and made notes so he could compare with what he was seeing on the study. And agreed that the study sounded like it would be inconclusive. Plan B: the ENT suggested we come home and use an at home pulse oxymeter to measure her oxygen saturation, overnight some night soon and video tape her sleeping. He will use these two pieces of evidence to draw his conclusions. He called tonight, having reviewed the study. He said her initial test she had 68 breath holding episodes an hour, with 5% of her sleep time spent under 90% blood oxygen saturation. This test showed 39 episodes an hour, with 7+% of her sleep spent under 90%. Better, but still not good. They expect to see <5 episodes an hour. He did see an improvement after the gauze was removed, but couldn't say whether it was the removing of the gauze or the addition of the oxygen. I could have told them that she was still having a significant number of breath holding episodes... even with the gauze removed, she still wasn't breathing normal. So, we will do our at home study once we settle back into our routine and Kaylee is sleeping well. It's going to be interesting to see the difference. |
 RSS Feed
RSS Feed